Implant Dental Lab
Choosing the right implant dental laboratory is a critical decision that directly impacts clinical outcomes, patient satisfaction, and the long-term reputation of your practice. The quality and consistency of your lab partner influence implant fit, occlusion, and overall case success. While many practices initially consider large corporate dental labs due to brand recognition, these operations often lack accountability and personalized communication, making it difficult to resolve complex cases or maintain consistency. At the opposite end, smaller labs may lack the advanced digital workflow, materials, or technical expertise required for modern implant dentistry, leading to variability in turnaround times and precision. The most effective approach is to work with a dental laboratory that balances technology, experience, and controlled case volume—ensuring consistent results, clear communication, and reliable implant restorations.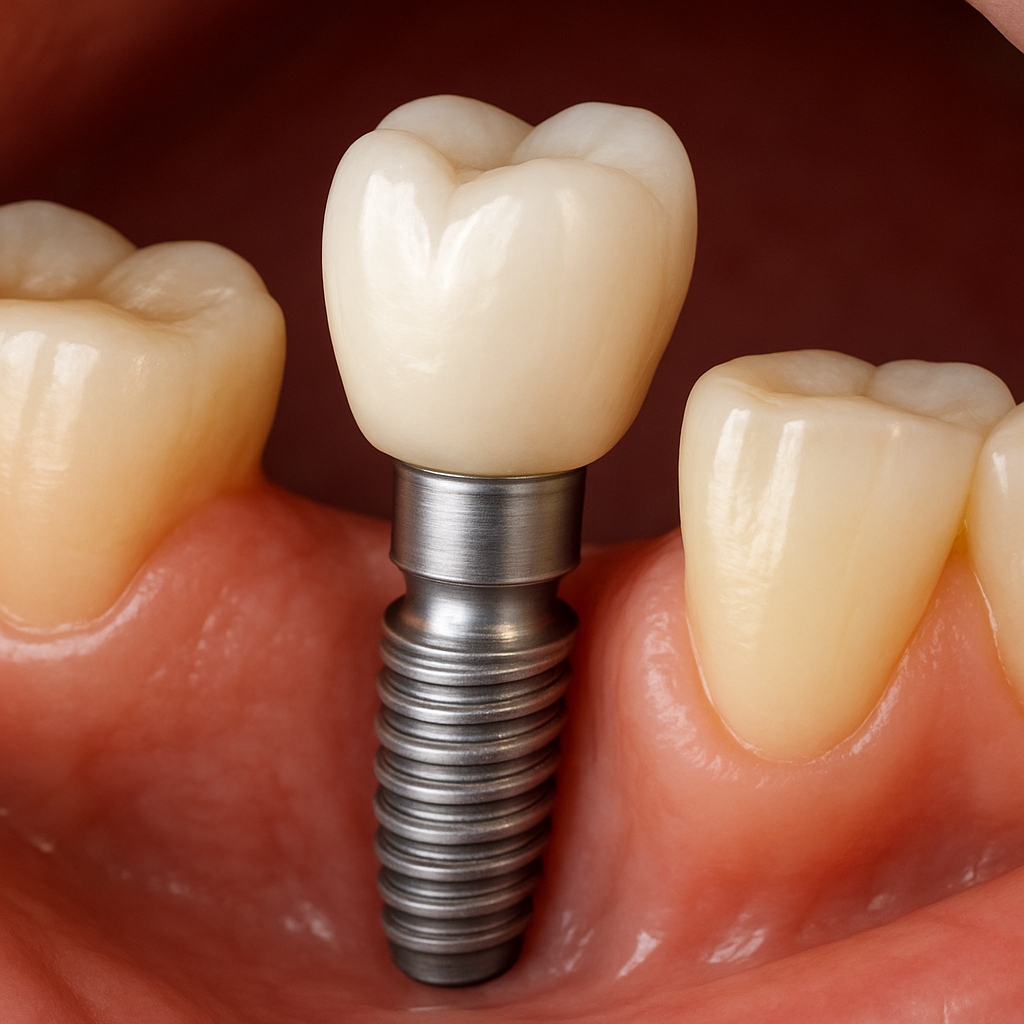
Medium-Sized, Owner-Operated Labs
When selecting an implant dental laboratory, a strategic approach is to work with a medium-sized, owner-operated lab that balances advanced technology with consistent oversight. These laboratories typically have the resources to invest in modern CAD/CAM systems and digital implant workflows while remaining responsive to the specific clinical needs of each practice. The Art of Aesthetics follows this model, combining digital precision with traditional craftsmanship, which is essential for complex implant restorations. Direct involvement from the owner and a stable team of technicians supports accountability, case continuity, and consistent results.
In contrast, large chain or franchise dental labs often rely on rotating technicians, which can introduce variability in communication, design preferences, and final outcomes. Without a dedicated technician familiar with your clinical expectations, implant cases may lack consistency from one case to the next. A dental laboratory operating under consistent leadership and controlled workflow provides predictable results, which is critical for maintaining clinical efficiency and patient trust.
Technology and Skill Go Hand in Hand
The success of an implant restoration depends not only on surgical precision, but also on the dental laboratory’s ability to deliver a prosthesis that fits accurately, functions properly, and meets esthetic expectations. A high-quality implant dental lab must combine advanced digital technology with experienced technicians. Modern workflows require intraoral scan compatibility, CAD/CAM design, and 3D printing to achieve precision and efficiency in implant restorations, including custom abutments and full-arch cases. However, technology alone is not sufficient. The final outcome depends on the technician’s ability to interpret clinical data, refine contours, and ensure proper occlusion and fit. A dental laboratory that integrates both digital capability and technical expertise will consistently produce predictable, high-quality implant results.
Avoiding the Pitfalls of Low-Cost Implant Dental Labs
While cost is always a factor, choosing the lowest-cost implant dental lab often leads to higher long-term risk. Many low-cost labs reduce pricing by outsourcing production, which can compromise quality control, material selection, and consistency. This frequently results in poor fit, occlusal issues, remakes, and increased chairside adjustments. If long-term clinical success and patient trust are priorities, selecting an implant dental laboratory based solely on price is not a sustainable strategy.
Communication and Collaboration with Your Implant Dental Lab
A strong working relationship with your implant dental lab depends on direct and effective communication. Complex implant cases often require discussion of implant positioning, emergence profile, occlusion, and material selection. Access to a knowledgeable technician or owner allows for accurate case planning and faster problem resolution. High-quality dental laboratories also support treatment planning by providing input on implant restorations, temporization, and final prosthesis design. This level of collaboration improves efficiency, reduces errors, and supports predictable outcomes.
Consistency and Customization in Implant Restorations
Consistency is critical in implant dentistry. Variations in contour, shade, or fit can disrupt clinical workflow and affect patient satisfaction. Larger labs often assign cases to multiple technicians, which increases variability. In contrast, a structured dental laboratory assigns a dedicated technician or team, allowing for better understanding of clinical preferences and implant systems. Over time, this leads to consistent, customized implant restorations with fewer adjustments. Customization also includes patient-specific factors such as tissue architecture, smile line, and functional dynamics.
Choosing the Right Implant Dental Lab Partner
The right implant dental laboratory combines advanced technology, skilled technicians, clear communication, and consistent workflow. A medium-sized, owner-operated lab provides the balance of capability and accountability required for modern implant dentistry. Selection should be based on accuracy, reliability, clinical support, and long-term consistency—not price alone. A strong lab partnership improves treatment outcomes, reduces complications, and enhances the overall patient experience.
Key to the Success of Dental Implant Restoration
Foundation First: Healing Cap Selection and Timing
The success of a dental implant restoration begins immediately after surgery. One critical factor often overlooked is the healing cap. Many clinicians default to a narrow healing cap, which can limit the emergence profile and compromise esthetics. Using a wider healing cap from the beginning better mimics natural tooth contours and supports proper soft tissue shaping. Preserving a broad gingival profile early reduces the risk of black triangles and recession while minimizing the need for future tissue manipulation.
Coordination with your implant dental lab is essential at this stage. The lab must understand your treatment plan and tissue objectives to design the restoration accordingly. The foundation established here directly influences the final outcome.
Material Selection: Matching Form to Function
Material selection plays a central role in the longevity and performance of implant restorations. Zirconia, lithium disilicate, and precious alloys each serve different clinical purposes. Zirconia provides strength for posterior restorations, while lithium disilicate offers superior translucency for anterior esthetics.
Abutment material is equally important. Titanium provides strength and biocompatibility for subgingival placement, while zirconia abutments are preferred in esthetic zones due to their color and tissue response. Material decisions must account for functional load, esthetic demands, implant system compatibility, and patient-specific factors such as bruxism.
Your implant dental lab should be involved in this decision-making process to ensure proper material selection and long-term success.
Retention Types: Cement vs. Screw-Retained Restorations
Choosing between screw-retained and cement-retained restorations is a clinical decision that directly impacts maintenance and long-term outcomes. Screw-retained crowns allow retrievability, easier maintenance, and reduced risk of peri-implant complications associated with excess cement. However, they require proper implant angulation and may present esthetic challenges in anterior cases.
Cement-retained restorations offer improved esthetics and flexibility. When properly managed with controlled margins or provisional cement, risks can be minimized. Flexibility in switching between retention types during treatment often leads to better results.
Close collaboration with your implant dental lab ensures both options are properly designed and executed.
Abutment Materials: Customization for Purpose
The abutment serves as the foundation of the final restoration. Titanium remains the standard for strength and durability, especially in posterior regions or patients with heavy occlusal forces.
In esthetic zones, custom zirconia or hybrid abutments provide improved emergence profiles and more natural color beneath translucent restorations. Custom abutments also allow precise margin placement and better soft tissue support, particularly in cases with thin biotypes or gingival asymmetry.
A qualified implant dental lab using digital design can fabricate abutments tailored to the implant system and tissue anatomy, reducing chairside adjustments and improving consistency.
Patient Education: Setting Realistic Expectations
Successful implant treatment requires clear patient communication. Patients must understand that implant restorations involve multiple stages, including healing, impressions, try-ins, and final delivery. This process may take several weeks or months and is essential for long-term success.
Esthetic expectations should also be addressed. Shade matching for implant restorations can be more complex than natural teeth. Patients may also experience an initial adjustment period as they adapt to the new restoration.
Working with a reliable implant dental lab helps manage expectations, reduce remakes, and improve patient satisfaction.
Digital Workflows and Lab Communication
Modern implant dentistry relies on digital workflows, including intraoral scanning, CAD/CAM design, and 3D printing. These technologies improve accuracy, efficiency, and turnaround time. Digital impressions eliminate traditional materials and allow immediate transfer of case data to the lab.
However, technology does not replace communication. Clear case instructions—including implant system, shade, occlusal clearance, and restoration type—remain essential.
A strong partnership with an implant dental lab ensures that digital tools are used effectively to deliver predictable outcomes.
Soft Tissue Management and Emergence Profiles
Soft tissue management is critical to the esthetic success of implant restorations. Healing caps, provisional restorations, and custom abutments all contribute to shaping the gingival contour.
A proper emergence profile should transition smoothly from the implant platform to the crown. Poor contour design can result in shadowing, food impaction, and hygiene challenges.
Working closely with your implant dental lab ensures that restorations support optimal tissue architecture from the early stages of treatment.
Final Crown Delivery: Details Make the Difference
At delivery, small details determine long-term success. Occlusion, proximal contacts, and margin fit must be carefully evaluated. Esthetics should be assessed under natural lighting to confirm shade, translucency, and surface texture.
A well-fabricated restoration from a qualified implant dental lab should require minimal adjustment, indicating accurate planning and execution.
Patient education on hygiene and follow-up care is essential to maintain long-term results.
The Success Equation in Implant Dentistry
Successful implant restorations result from careful planning, precise execution, and clear communication among clinician, lab, and patient. Every step—from healing cap selection to final delivery—contributes to long-term function and esthetic success.
Material selection, retention strategy, and abutment design must align with the clinical situation. Partnering with a skilled implant dental lab ensures consistency, accuracy, and predictable outcomes.
Discussing the Benefits of Leading Implant Brands
Straumann: Precision and Global Trust
Straumann is a globally recognized implant system known for precision, innovation, and long-term reliability. Its implant designs support strong osseointegration and consistent clinical outcomes. Straumann also offers a highly integrated digital ecosystem, allowing seamless compatibility with intraoral scanners and CAD/CAM systems. This improves communication with your implant dental lab and enhances workflow efficiency. The combination of scientific validation, digital capability, and restorative flexibility makes Straumann a preferred choice for clinicians focused on consistency and quality.
Nobel Biocare: Immediate Function and Proven Systems
Nobel Biocare is widely regarded as a pioneer in implant dentistry, particularly in immediate loading protocols. Its systems are backed by extensive clinical research and precision engineering. Nobel’s Procera CAD/CAM platform supports customized abutments and efficient communication with your implant dental lab. For practices seeking predictable outcomes with streamlined workflows, Nobel Biocare remains a reliable and well-established option.
Azure: Modern Design with Competitive Value
Azure is an emerging implant brand offering modern design features at a more accessible price point. Its systems incorporate platform-switching and conical connections to improve stability and preserve crestal bone. Azure implants are compatible with major digital workflows, allowing smooth integration with your implant dental lab. While newer to the market, Azure provides a balance of performance, affordability, and digital flexibility for practices managing cost without compromising function.
Encode Healing Abutments: Digital Efficiency in Restorative Workflow
Encode by Zimmer Biomet simplifies the restorative process through digitally encoded healing abutments. These components eliminate the need for traditional impressions by allowing intraoral scanning directly from the healing abutment. This reduces chair time, improves patient comfort, and enhances accuracy. The ability to transmit data directly to your implant dental lab streamlines case processing and supports predictable outcomes, particularly in single-unit restorations.
Atlantis: Customized Abutments for Esthetic Precision
Atlantis, part of Dentsply Sirona, specializes in patient-specific abutments designed using CAD/CAM technology. Each abutment is customized based on implant position and soft tissue anatomy, improving emergence profile and esthetic integration. Material options include titanium, gold-shaded titanium nitride, and zirconia, allowing flexibility across clinical scenarios. These custom solutions improve long-term stability and reduce chairside adjustments when coordinated with your implant dental lab.
BioHorizons: Biologic Design and Tissue Stability
BioHorizons is known for its Laser-Lok surface technology, which promotes soft tissue attachment and bone preservation. This biologically driven design improves implant stability and long-term tissue health. The system also features simplified restorative workflows and compatibility with digital platforms. BioHorizons works efficiently with implant dental labs to ensure precise component matching and timely case completion.
Astra Tech: Long-Term Clinical Performance
Astra Tech, under Dentsply Sirona, is supported by extensive long-term clinical studies. Its implant systems focus on maintaining peri-implant tissue health and ensuring long-term stability. Astra integrates seamlessly with custom abutment systems such as Atlantis, allowing efficient collaboration with your implant dental lab. It is often selected in cases where long-term predictability is a primary concern.
Zimmer Biomet: Versatility and Digital Integration
Zimmer Biomet offers a broad range of implant solutions designed for versatility and ease of use. Its Tapered Screw-Vent system provides strong primary stability and reliable performance across different clinical scenarios. Integration with the Encode system allows direct digital communication with your implant dental lab, eliminating traditional impression steps. This improves turnaround time and enhances accuracy in restorative outcomes.
Connecting an Implant Abutment with a Natural Abutment
Why This Approach Is Rare
Connecting a natural tooth to an implant is generally avoided due to biomechanical differences. Natural teeth move under load, while implants remain rigid. This mismatch can lead to uneven force distribution, increasing the risk of complications such as screw loosening or bone loss.
When It Becomes Necessary
In certain clinical situations—such as limited bone or long-span edentulous spaces—connecting a tooth and implant may be unavoidable. These cases require advanced planning and close coordination with your implant dental lab to ensure stability and function.
Managing Biomechanical Risks
To compensate for movement differences, stress-breaking designs such as telescopic copings are often used. These systems help distribute forces more evenly and reduce stress on the implant.
Telescopic Copings Explained
Telescopic copings consist of a primary coping on the natural tooth and a secondary coping within the prosthesis. This design allows controlled movement and improves long-term function. Precision fabrication by an implant dental lab is essential to ensure proper fit and performance.
Case Example: Unilateral Mandibular Posterior Restoration
Imagine a patient missing mandibular molars on one side, with a single canine remaining anteriorly. Bone grafting is not possible due to anatomical constraints, and only one implant can be placed in the first molar region. To restore proper occlusion and function, the clinician chooses to splint the implant with the canine. A telescopic coping is placed over the canine, and a fixed bridge connects it to the implant-supported crown. The primary coping is cemented, and the secondary coping is part of the bridge. Because the system allows slight vertical movement of the natural tooth without stressing the implant, it preserves both components.
This strategy wouldn't be possible without digital design collaboration with a skilled implant dental lab. The lab must ensure parallelism, margin accuracy, and a passive fit of the final bridge, all while balancing the aesthetic and functional needs of the patient.
Material Considerations for Longevity and Precision
Choosing the correct material for telescopic copings is essential. Gold alloys are known for their wear resistance and excellent marginal fit. The internal surface of the secondary coping must allow smooth insertion and removal without creating pressure points. This is particularly important if the coping is being used in a semi-removable prosthesis. Any frictional resistance must be consistent and reproducible. Because of the need for micron-level accuracy, working with an implant dental lab that has CAD/CAM capabilities is crucial. Labs must use digital scanning, milling, and verification techniques to ensure a precise and passive fit.
Limitations and Contraindications
Although telescopic systems provide a solution in challenging cases, they're not suitable for every patient. Mobility of the natural abutment, periodontal compromise, or insufficient crown height space can make telescopic connections unreliable. Additionally, patient compliance is critical. Hygiene must be impeccable, and periodic evaluations are necessary. If the patient cannot return for regular maintenance or struggles with removable prostheses, alternative treatment plans should be considered.
Collaboration Is Key in Complex Cases
Connecting a natural abutment to an implant abutment is not standard practice and should be reserved for exceptional cases. When no better alternative exists, telescopic copings provide a biomechanically sound and patient-friendly solution. These restorations require interdisciplinary planning, digital precision, and extensive collaboration with a skilled implant dental lab. By leveraging the strength of telescopic designs and understanding their limitations, clinicians can offer patients a viable solution where traditional fixed options fall short. Ultimately, success comes not just from materials or implants, but from communication, customization, and clinical judgment.
What's the Best Crown Material for Implant Restoration?
Understanding Crown-Abutment Combinations in Implant Dentistry
Choosing the right crown material for an implant restoration is essential to ensure durability, aesthetics, and patient satisfaction. Unlike natural teeth, implants lack a periodontal ligament and cannot accommodate minor stress or movement. Therefore, material selection must consider not only visual outcomes but also functional longevity and biomechanical compatibility. The abutment serves as the foundation between the implant and the crown. As such, different combinations of abutment and crown materials are tailored based on the restoration location, aesthetic demands, and occlusal forces.
Each pairing has unique benefits and limitations that clinicians must understand to make the best choice. Coordination with an experienced implant dental lab ensures the proper fit, material handling, and contouring for optimal results.
Titanium Abutment + PFM Crown: The Time-Tested Classic
A customized titanium abutment paired with a porcelain-fused-to-metal (PFM) crown is a reliable and long-standing solution. Titanium offers exceptional strength, biocompatibility, and long-term resistance to corrosion. Its mechanical properties make it ideal for posterior restorations where chewing forces are strongest. PFM crowns, consisting of a metal substructure layered with porcelain, provide reasonable aesthetics while maintaining durability. The porcelain surface mimics tooth-like translucency, although it may not be as lifelike as zirconia layered or e.max crowns. Nevertheless, PFM crowns are less brittle than full ceramic options and withstand chipping better under load. Also, block out metal underneath the crown.
This combination is suitable for molars, where aesthetics are secondary, but strength and longevity are crucial. Moreover, this pairing can be more cost-effective than high-end ceramics. The collaboration with an implant dental lab ensures that the metal substructure doesn't compromise soft tissue contours or esthetic margins. However, the potential for metal shine-through in thin tissue should be taken into consideration.
Titanium Abutment + Monolithic Zirconia Crown: Strength Meets Simplicity
A customized titanium abutment with a monolithic zirconia crown is one of the most popular modern combinations for implant restorations. This pairing offers unmatched strength and fracture resistance, making it ideal for bruxers or high-load posterior regions. Monolithic zirconia is milled from a single block, eliminating the weak points associated with layered ceramics. It resists wear and rarely fractures. Although early versions were opaque and less aesthetic, newer generations of translucent zirconia have improved dramatically in mimicking natural tooth color.
This solution is preferred when both durability and moderate aesthetics are desired. Because the titanium abutment ensures precise fit and support, the monolithic crown functions efficiently without the risk of chipping or delamination. However, it's not ideal for anterior shade and aesthetic matching.
Full Zirconia Abutment + Layered Zirconia Crown: Esthetics with a Caution
Using a customized full zirconia abutment paired with a zirconia crown layered with porcelain offers high aesthetic value. This combination is commonly used in the anteriors, where patients expect a seamless blend with natural teeth. Zirconia abutments are tooth-colored and promote better soft tissue response than metal. They prevent grayish discoloration of the gingiva, especially in thin biotypes. Layering the zirconia crown with feldspathic or porcelain powder allows for incredible translucency and detail. However, full zirconia abutments are not as strong as titanium. They are prone to fracture under high stress or poor angulation. This limits their use to carefully selected cases where the bite is minimal and implant positioning is ideal.
Due to the fragility of the components, precision fabrication is crucial. Your implant dental lab must ensure a passive fit, a perfect emergence profile, and strong bonding between the abutment and crown. When executed flawlessly, this combination offers the most lifelike restoration available.
Zirconia-Titanium Hybrid Abutment + Layered Zirconia Crown: Best of Both Worlds
The zirconia-titanium hybrid abutment with a layered zirconia crown represents a modern and balanced solution. It combines the strength of titanium with the soft tissue compatibility and aesthetics of zirconia. This dual-component abutment consists of a titanium base that interfaces with the implant and a zirconia sleeve that supports the crown. This approach eliminates the risk of zirconia fracture at the implant interface while still allowing a natural-looking emergence from the gingiva. The layered zirconia crown enhances aesthetics with its hand-applied porcelain, giving it depth, translucency, and character.
Clinicians often choose this combination for most implant restorations where both strength and aesthetics are important. The titanium base ensures secure implant integration, while the zirconia portion maintains a pleasing appearance under soft tissues. An experienced implant dental lab plays a critical role in bonding the hybrid abutment, designing ideal contours, and managing translucency during porcelain layering. When done correctly, this solution maximizes performance and appearance.
Titanium Abutment + Full Gold Crown: Longevity and Function with a Cost Caveat
Gold crowns have long been the gold standard (literally) for durability and biocompatibility. When paired with a custom titanium abutment, a full gold crown offers unmatched longevity and adaptability. Gold is soft enough to adapt precisely to opposing teeth, reducing wear and improving occlusal harmony. Because of its malleability and excellent marginal seal, gold is especially suitable for patients with high bite forces or parafunctional habits. Titanium ensures a stable, corrosion-resistant foundation, making this combination one of the most mechanically reliable choices.
However, gold is significantly more expensive than other materials. Its aesthetics are also a major limitation—most patients are unwilling to accept a visible gold crown in the anterior or premolar. Despite these drawbacks, the titanium abutment plus gold crown option remains ideal for posterior molars, especially when longevity is the top concern. An implant dental lab with experience in precious metal casting ensures that both fit and finish are optimal for the clinical situation.
Matching Crown Materials to Clinical Priorities
The ideal crown material isn't universal—it depends on the patient's specific needs. Factors like aesthetic expectations, occlusal bite, implant angulation, tissue biotype, and even financial constraints all influence the decision. Choosing a crown-abutment combination should reflect both clinical reasoning and patient preference. For example, a young patient with high aesthetic expectations may benefit from a hybrid abutment and layered zirconia crown. Meanwhile, an elderly bruxer needing a second molar restored would be better served with a monolithic zirconia or gold crown over a titanium abutment.
Regardless of the combination, collaboration with a qualified implant dental lab ensures consistency in material handling, design accuracy, and esthetic execution. Digital scans, shade matching, and custom contouring contribute to seamless integration and clinical success.
Digital Planning and CAD/CAM Precision
The growing role of digital workflows cannot be overlooked when selecting crown materials. Many modern abutments and crowns are designed using CAD/CAM systems, improving accuracy, reproducibility, and turnaround times. Custom abutments, whether titanium, zirconia, or hybrid, can be digitally planned to optimize emergence profiles, soft tissue support, and cement margins. Similarly, crown designs can be fine-tuned digitally before milling or layering. To summarize, no single crown-abutment combination suits every case. The best solution is one that meets both clinical requirements and patient expectations while minimizing long-term risks.
Here are some clinical tips to guide your decision:
- Use titanium abutments in heavy bite or when strength is a priority.
- Reserve full zirconia abutments for low-stress and aesthetic cases.
- Consider hybrid abutments and zirconia layered crowns that demand both beauty and strength.
- Layered IPS e.max crowns offer superior aesthetics but may require more careful handling, best for anterior shade matching.
- Monolithic zirconia and gold are preferred when durability and function outweigh appearance.
- Partnering with a lab that understands these nuances ensures that you get not only a crown that fits but one that lasts.
Preparing Your First Case with The Art of Aesthetics Implant Dental Lab
Understanding the Relationship You're Entering
When you decide to work with The Art of Aesthetics, you're entering a premium partnership, not just outsourcing a case. Unlike high-volume, corporate-style labs, we pride ourselves on individualized craftsmanship and long-term collaboration with full-time dental professionals. To ensure a smooth start, there are several essential guidelines you must follow before sending your first case.
Please note, we are not a high-throughput, budget-driven lab. Our clients choose us because we consistently deliver quality and customization. Building that relationship takes time, communication, and commitment. If you're looking for a fast or one-time solution, we are likely not the right fit.
We strongly encourage every new client to read through our process and understand what working with a boutique implant dental lab like ours entails. This foundation ensures mutual respect and clinical success.
Read Our Terms and Conditions Thoroughly
Before you send us any components or case instructions, please take the time to review our Terms and Conditions carefully. These terms outline everything from delivery timelines to liability, communication protocols, remakes, and case rejection policies.
These guidelines are not mere formalities—they protect both you and our technicians. We hold ourselves to the highest standards, but we also require clarity and commitment from our clients. Your acknowledgment of our policies allows us to prioritize your cases with confidence. If any part of the terms is unclear, we welcome your questions. Clear expectations from the start prevent misunderstandings later. Our goal is to collaborate, not simply fulfill orders. Each implant dental lab operates with its own protocols. Knowing ours upfront puts your case on a smoother track from day one.
Send Complete Implant Information—Every Time
A successful restoration depends on detailed and accurate information. Before we begin, you must send all relevant implant details, including:
- Implant brand and platform
- Type of abutment requested
- Healing cap or scan body (if applicable)
- Gingival height and emergence profile preferences
- Desired retention type (cemented or screw-retained)
- Restoration material selection (zirconia, PFM, etc.)
- Photographs or shade guide references
- Occlusal scheme and bite records
We cannot proceed with incomplete submissions. Missing data delays workflow and compromises quality. If we receive a case without key components or clarity, we will place it on hold until all materials are provided. The Art of Aesthetics Implant Dental Lab functions as an extension of your clinic. Without the full picture, we cannot perform at our best.
Quality Takes Time—Especially for the First Case
Every dentist has unique preferences. From margin preference to occlusal design, we learn your expectations case by case. The first restoration takes longer because we prioritize accuracy over speed. Please allow a 3–5 week turnaround from the time we receive all components and information. This window includes time for model scanning, digital design, technician consultation, fabrication, and quality assurance. The first case always requires more back-and-forth as we establish your settings and nuances.
Rushing this process only leads to errors and dissatisfaction. We'd rather get it right the first time than deliver a remake later. Once your preferences are established, future cases will move faster and more efficiently. Your patience during this initial learning phase allows us to provide you with a higher level of care. Many corporate labs may work faster, but they do so at the expense of consistency and communication. That's not how we operate at our implant dental lab.
We Only Serve Regular, Full-Time Clinicians
We intentionally limit the number of clients we serve to maintain our standards. As such, we do not accept one-time or emergency-only cases. Our goal is to build long-term partnerships, not accommodate temporary needs when other labs say no. If you're looking for a quick fix or have been turned away elsewhere, we encourage you to explore other providers. Our success comes from sustained collaboration with clinicians who value precision, communication, and shared responsibility.
This exclusivity ensures that our full-time clients receive undivided attention. Each implant dental lab must decide how to allocate its resources—we choose quality over quantity, always.
We Use Only Premium Brands and Proven Systems
Our lab does not use generic or off-brand implant parts. If you prefer a restoration that involves third-party components or cost-cutting systems, we cannot be held responsible in this case. We specialize in high-quality brands such as Straumann, Nobel Biocare, Astra Tech, BioHorizons, Zimmer Biomet, and similar platforms. This is not a matter of preference—it's about ensuring fit, compatibility, and predictable outcomes. Lower-cost parts often lack manufacturing precision, which increases chairside adjustment time and risk of failure. Furthermore, they may be incompatible with digital workflows or present safety concerns over time.
Partnering with a premium implant dental lab means committing to premium materials. If saving money is your top priority, we are not the lab for you. Our clients seek predictability and performance, not shortcuts.
It Takes Multiple Cases to Learn Your Preferences
We urge you not to judge our work based on a single case. A strong lab-clinic relationship forms over time. Subtle preferences—like occlusal contact points, pontic contouring, or shade selection—become more refined with each case. The first few restorations are about calibration. We learn from your feedback, and you learn how we interpret your instructions. With every case, we improve the alignment between your expectations and our production. If you're unsure whether we're a good fit, we recommend sending at least five to ten trial cases. After that, you'll have a clearer picture of our capabilities and consistency.
Every implant dental lab strives for excellence, but excellence isn't built overnight. We ask for your investment in the learning process, and in return, we commit to continuous improvement and communication.
Final Thoughts: Begin withIntention, Not Urgency
If you're considering sending your first case to The Art of Aesthetics Implant Dental Lab, we invite you to approach it thoughtfully. Review the expectations. Prepare your documentation thoroughly. Understand that we are building something long-term, not a one-time transaction. A high-end implant restoration is a collaborative effort between the dentist and the lab. The more intentional you are, the better your outcomes will be.
We are not simply providing products—we're contributing to patient care alongside you.
Begin this journey with the understanding that great things take time, care, and alignment. Our team is here not just to fabricate, but to partner, improve, and elevate your implant dentistry.